"It’s great to use this medicine!"
In 2022, on the first day of the new year, in the inpatient department of neurology of Henan Children’s Hospital, a child with congenital spinal muscular atrophy (SMA) less than 3 years old was being treated by injection of Nocicnatrium.
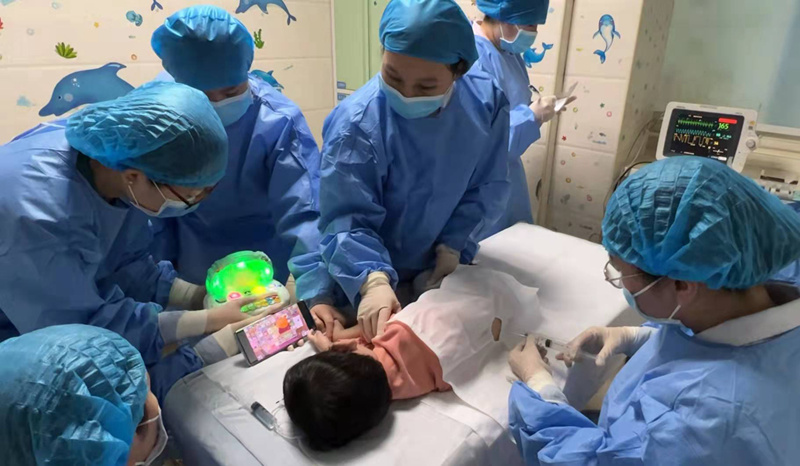
The child is being treated with Nocicnatrium injection. Photo courtesy of Henan Children’s Hospital
From nearly 700,000 to tens of thousands of yuan, Nocicnatrium injection entered the medical insurance, which greatly reduced the burden of medical treatment for children. "This can cure the disease, and the child has hope." The words of the child’s mother reveal a beautiful vision for the future.
And this is just a microcosm of China’s people’s sense of gain in the field of medical insurance. On March 6th, 2021, General Secretary of the Supreme Leader visited the members of medical and health circles and education circles who attended the Fourth Session of the 13th Chinese People’s Political Consultative Conference, and participated in the joint meeting to listen to opinions and suggestions. He stressed that it is necessary to continue to intensify the reform of medical insurance, normalize and institutionalize the centralized procurement of drugs, improve the medical insurance and assistance system for serious and serious diseases, deepen the reform of the supervision system of medical insurance funds, and keep the people’s "life-saving money" and "life-saving money".
In 2021, the reform in the field of medical insurance was unprecedented, the burden of drug consumption was significantly reduced, the experience of medical treatment in different provinces was steadily improved, and the "medical money" and "life-saving money" were safer. In order to meet the people’s more expectations, China is writing more warm "healthy answers" with the pen of innovation.
The effect of "combined price reduction" released the burden of people’s medication and continued to reduce.
"Every small group should not be abandoned."
"It’s really hard. In fact, just now I felt that my tears were about to fall."
— — Zhang Jinni, Negotiator of National Medical Insurance Bureau and Director of Medical Equipment Procurement Supervision Department of Fujian Medical Insurance Bureau.

On November 11, 2021, the medical insurance catalogue negotiation site. Cctv screenshot
At the end of 2021, a video of the national medical insurance catalogue drug negotiation site was circulated on the Internet. After two rounds of nine negotiations by the medical insurance department, the price of Nocicnatrium injection was finally sold at the price of tens of thousands of yuan per needle. Previously, the drug was called "high-priced drug" because its price per injection was 699,700 yuan, and patients needed to inject 4 injections in the first 63 days and 1 injection every 4 months thereafter, which was expensive for life.
In order to let the people use good drugs with high quality and low price, since the establishment of the National Medical Insurance Bureau in 2018, the list of medical insurance drugs has been dynamically adjusted once a year for four consecutive years, and a total of 507 new drugs and good drugs have been included in the list, and patients’ medical treatment and drug use are increasingly guaranteed.
In 2021, on the basis of increasing innovative drugs and anti-tumor drugs, the "zero breakthrough" of bringing high-value drugs for rare diseases into medical insurance was realized. Li Tao, deputy director of the National Health Insurance Bureau, said that in 2021, seven rare disease drugs were successfully negotiated, with an average price drop of 65%.
At the same time, the centralized procurement of drugs is gradually normalized and institutionalized. Since the centralized procurement of drugs in the "4+7" pilot city was opened in Shanghai in December 2018, the Office of Joint Procurement of Drugs organized by the State has organized six batches and seven rounds of national centralized procurement. The average price of drugs and consumables was reduced by more than 50% and 80% respectively, thus reducing the burden on the masses by more than 250 billion yuan.
In March this year, the varieties of artificial total knee joint and artificial total hip joint will also land nationwide, with an average price reduction of 82%. It is estimated that it will benefit nearly 11 million patients and reduce the burden by nearly 30 billion yuan every year.
"Under the principle of safety, effectiveness and economy, in 2021, the medical insurance catalogue will be adjusted to include more drugs with high quality and low price, and at the same time, the centralized procurement of drugs has become normal. Through centralized procurement and catalogue access negotiations ‘ Combination boxing ’ Significantly reduced the burden of medication for the masses. " Wang Zhen, a researcher at the Institute of Economics of China Academy of Social Sciences, said in an interview with People’s Daily.
Direct settlement of medical treatment in different places makes reimbursement no longer "running around"
"Usually, there is a headache and brain fever. You only need a little mobile phone to complete cross-provincial reimbursement."
In order to take care of her granddaughter, Aunt Han came to Beijing from Shanxi, more than 600 kilometers away. She praises everyone, and now it is really convenient to use the medical insurance service platform APP for reimbursement. You can also switch the "Care Edition", which makes the operation easier.
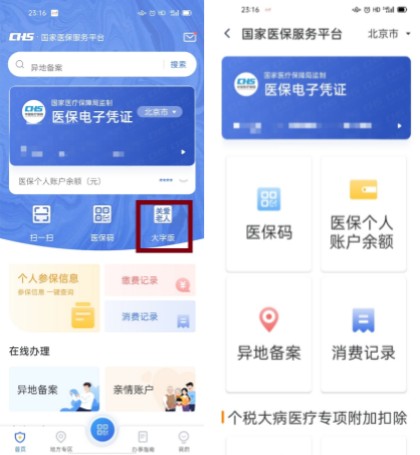
The national medical insurance service platform APP launched a "caring version" to facilitate the elderly. Screenshot of the national medical insurance service platform APP
In recent years, with the large increase of people living in different places, retiring in different places and working in different places, especially the growing number of elderly people moving with their children, there is a higher demand for direct settlement of medical treatment in different places.
Focus on the medical settlement needs of the 125 million inter-provincial floating population, and further promote the "streamline administration, delegate power, strengthen regulation and improve services" reform in the field of medical insurance. Since 2021, the National Medical Insurance Bureau has consolidated and expanded the results of inter-provincial direct settlement of hospitalization expenses, and comprehensively promoted the inter-provincial direct settlement of outpatient expenses.
At present, the cross-provincial direct settlement service for hospitalization expenses in different places has covered all provinces, all overall planning areas, all kinds of insured persons and main out-going personnel in China, and 52,900 designated medical institutions have been connected to the network, basically achieving the goal of full coverage of designated hospitals and at least one designated hospital in each county.
At the same time, the direct settlement of general outpatient expenses across provinces was accelerated. From fully opening the pilot areas of Beijing-Tianjin-Hebei, Yangtze River Delta and Southwest China, to adding 15 provinces including Shanxi as pilot provinces, the regional pilot has turned to full implementation. By the end of November 2021, all provinces and Xinjiang Production and Construction Corps have started direct inter-provincial settlement of general outpatient fees, covering 97.6% of the country’s overall planning areas, with more than 120,000 networked designated medical institutions and at least one networked designated medical institution in 91.7% of the counties.
"From the current situation, there are no institutional and policy obstacles in direct settlement of medical treatment in different places, whether it is outpatient or inpatient." According to Wang Zhen’s analysis, from the management of medical insurance fund, there are no problems such as the rapid increase of medical expenses in different places and the influence of medical order after direct settlement, which is due to the refined management of direct settlement of medical treatment in different places and the construction of information system.
Ying Yazhen, vice president of the National Medical Insurance Research Institute and vice president of the China Medical Insurance Research Association, said that the main progress in promoting the settlement of medical insurance in different places is as follows: the cross-provincial direct settlement system for hospitalization expenses covering the whole country is running smoothly and becoming increasingly mature; The number of effective filing of national platforms is increasing, and the benefits are expanding; Carrying out medical insurance settlement in different places is conducive to promoting the standardization of medical insurance; It is conducive to gradually improving the overall level of medical insurance.
"Now, there are still some technical problems. For example, there are still blocking points in the direct settlement of outpatient clinics, and some medical institutions that have been connected still have problems in the actual settlement process." Wang Zhen suggested further opening up the information system and improving the flexibility and convenience of filing.
"It is also necessary to strengthen the connection and cooperation between the medical insurance policy and the handling management between the insured place and the medical treatment place, and between the medical insurance departments. In particular, it is necessary to strengthen joint supervision, prevent excessive medical treatment in the process of medical treatment in different places, and ensure the safety of the medical insurance fund." Ying Yazhen stressed.
The reform of payment method helps the "medical insurance patients" win-win situation.
In the speech contest of medical reform experience held in Sanming City, a dean told a story of two invoices: "The same two hospitalization invoices of 30,000 yuan, 70% at their own expense 10 years ago, reimbursed 30%, and the patient spent 21,000 yuan; After 10 years, he paid 30% at his own expense and reimbursed 70%. The patient spent 9,000 yuan. " — — Sanming, Fujian, is known as one of the cheapest places for ordinary people to see a doctor in China.
For a long time, the traditional medical insurance payment method in China is to pay by project, that is, according to all drugs, medical services and medical consumables used in the diagnosis and treatment process, how much the hospital uses in the diagnosis and treatment process, and how much the medical insurance and patients pay according to the proportion. Under this model, excessive medical behaviors such as "big prescription" and "big examination" may occur, which not only wastes medical resources, but also makes the insured spend more money and the medical insurance fund spend more.
In 2017, Sanming was selected as one of the three pilot cities in the country’s "C-DRG reform", and for the first time nationwide, medical insurance and patients and hospitals were settled according to the quota of diseases at the same time, and there was no deductible line. The medical insurance fund was reimbursed 70% and 80% according to the quota of diseases, and the individual out-of-pocket payment was 30% and 20% respectively. Through the reform, medical institutions at the same level, urban workers and urban and rural residents have achieved "the same disease, the same treatment, the same homogeneity and the same price".

Medical reform publicity column in front of Youxi County General Hospital in Sanming City, Fujian Province. People’s Daily reporter Yang Di photo
The effect of the reform is obvious. In 2020, there were 229,600 cases discharged from medical institutions at or above the county level in Sanming, of which 187,300 cases were settled according to DRG, and the enrollment rate reached 81.58%. The balance of medical insurance fund was 69.71 million yuan according to the quota of diseases, which effectively reduced the medical cost.
Summing up Sanming’s experience, Fujian Province, based on its own actual situation, explored a reform road of "Pay by Disease Score (DIP)" by using big data technology, and promoted the development of medical insurance along the track of high quality and refinement.
On the basis of the previous pilot, the National Medical Insurance Bureau launched two new payment models, DRG and DIP, at the end of 2019 and 2020. As of October 2021, the actual payment of DRG in 30 pilot cities has covered 807 medical institutions.
"The reform of DRG/DIP payment method highlights value medical care, which is bound to have an impact on hospitals, medical insurance and patients." Wang Zhen analyzed to reporters that in the hospital, the operating mechanism under the previous project payment was changed, from "seeing a doctor" as the center to patient health as the center; From seeing a doctor more, the more money you make, and gradually to the healthier the patient, the more money you make. In terms of medical insurance, it has shifted from project management to "value" management, and post-supervision has shifted to supervision before, during and after the event. In terms of patients, it reduces the burden of medical treatment and improves the quality of diagnosis and treatment.
At the end of November, 2021, the National Health Insurance Bureau issued the "Three-year Action Plan for the Reform of DRG/DIP Payment Method", aiming at accelerating the establishment of an effective and efficient medical insurance payment mechanism and accelerating the reform by stages. According to the plan, by the end of 2025, DRG/DIP payment method will cover all eligible medical institutions that provide hospitalization services, and basically achieve full coverage of diseases and medical insurance funds.
"This is a win-win and mutually beneficial reform for the three parties of medical insurance patients." Ying Yazhen commented.
Find out the fraud, cheat the "Shuo" and keep the people’s "life-saving money"
Up to 70-year-old people and down to 5-year-old children, why do more than 2,000 villagers in the village collectively "suffer" from a stroke? — — In October last year, a report caused public outcry.
Stroke is neither an infectious disease nor an endemic disease, but in Cuikou Village, Laihe Town, Shan County, Heze City, Shandong Province, many villagers’ medical insurance accounts have inexplicably recorded many strokes in the past five years. Immediately, the National Medical Insurance Bureau sent a working group to Shan County for on-site supervision.
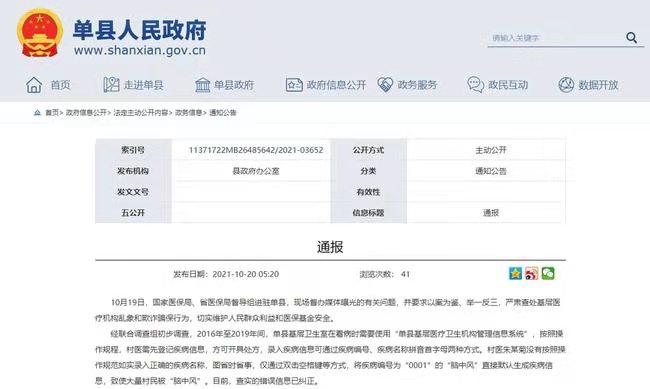
Shanxian County, Heze City, Shandong Province reported "stroke in the whole village". Screenshot of official website of Shan County People’s Government
In fact, such as the case of medical insurance fraud in Shanxian County, it is not a case. There are still many "shuoshu" in the idea of "saving money" for the people.
According to the data of the National Medical Insurance Bureau, from 2018 to October 2021, the National Medical Insurance Bureau and other relevant departments recovered about 50.6 billion yuan of medical insurance funds. In 2021, the National Medical Insurance Bureau exposed 58 typical cases in batches. Only the latest batch of typical cases involved more than 12 million yuan of fraudulent medical insurance funds, and the regulatory situation was severe and urgent.
In order to strengthen the supervision of the use of medical insurance funds and effectively safeguard the safety of medical insurance funds, in early 2021, the State Council promulgated the first regulation on medical insurance supervision in China, the Regulation on the Supervision and Administration of the Use of Medical Insurance Funds, which changed the situation that there is no special law in the field of medical insurance in China.
Subsequently, the Interim Measures for the Fixed-point Management of Medical Insurance in Medical Institutions, the Interim Measures for the Fixed-point Management of Medical Insurance in Retail Drugstores and the Measures for Standardizing the Discretion of Administrative Punishment in the Use, Supervision and Management of Medical Insurance Funds were successively implemented, which provided the basis and support for the medical insurance department to carry out fund supervision.
In order to strengthen the convergence of execution of medical insurance fund cases, in November 2021, the National Medical Insurance Bureau and the Ministry of Public Security jointly issued the Notice on Strengthening the Convergence of Execution in Investigating and Handling Cases of Deceiving Medical Insurance Fund, and put forward specific requirements and practices.
By severely cracking down on violations of laws and regulations in the field of medical insurance, in 2021, the national medical insurance department inspected 708,000 medical institutions, handled 414,000 times, recovered more than 23 billion yuan, and exposed 70,000 cases.
What are the difficulties in eradicating medical insurance fraud? Jin Weigang believes that it is mainly reflected in several aspects: the medical insurance fund has a huge expenditure and the losses caused by fraud are expanding; With the improvement of medical insurance benefits, the proportion of patients’ personal payment decreases, the sensitivity to medical expenses decreases, and the opportunity for criminals to commit fraud increases; The number of insured persons has increased greatly, and the composition of personnel is complex, so it is difficult to monitor the medical treatment behavior of insured persons; Grass-roots medical institutions are loosely managed, so it is difficult to supervise their medical service behavior.
In the face of the above situation, how to maintain the safety of medical insurance fund? Jin Weigang said that it is necessary to treat both the symptoms and the root causes and constantly improve the anti-fraud mechanism of medical insurance. Strengthen the construction of medical insurance legal system, including perfecting the relevant laws and regulations system, and clearly define the provisions of severe punishment for medical insurance fraud from three levels: administrative punishment, civil liability and criminal liability; Take targeted anti-fraud measures, such as improving the medical insurance information system and developing and popularizing a professional medical insurance fraud identification system; Establish a special medical insurance anti-fraud agency and equip it with corresponding professionals.
In addition, Wang Zhen also suggested that the regulatory measures should be updated first. "The magic height is one foot" and "the road height is one foot", especially for the new type of fraud and insurance fraud, it needs new high-tech supervision means based on modern information technology; Secondly, we should improve the multi-department linkage mechanism and strengthen the linkage mechanism with the commission for discipline inspection, public security, health care, market management and other departments; It should also be combined with reform measures such as payment method reform and centralized drug procurement to improve supervision methods.
At present, the reform of China’s medical insurance system is still advancing. Standing at the beginning of the new year, people are expecting more "explosive materials" for reform. China’s medical security network is becoming more and more dense around strengthening the security capacity and reducing the burden on the masses.